Problems with the current USA health care system
- Poor overall results, compared to most other developed countries:
lower life-expectancy, higher costs, higher infant mortality, etc.
Commonweatlh Fund's "Mirror, Mirror 2021: Reflecting Poorly"
"The cost of a long life" chart (from UCSC's "Health Care Spending")
Reuters "U.S. scores dead last again in healthcare study" (2010)
Lenny Bernstein's "Once again, U.S. has most expensive, least effective health care system in survey" (2014)
New York Times "Health Spending vs. Results"
Tyler Heymans' "Why The American HealthCare System Sucks"
Life-expectancy only: Matthew O'Brien's "The Singular Waste of America's Healthcare System in 1 Remarkable Chart" - High costs.
Alleged causes:- Uninsured:
- No care until their condition changes from mild to severe.
- Get care in an expensive ER instead of in a doctor's office.
- High cost of drugs and medical devices.
- High salaries of doctors.
Matthew Yglesias' "Doctors Fire up the Obamacare Waaambulance" - Pay-per-procedure or pay-per-time instead of pay-for-results.
- Litigation, and cost of malpractice insurance.
- Costs added by insurance companies:
- Company costs: profit, high executive salaries, advertising, lobbying, lawyers.
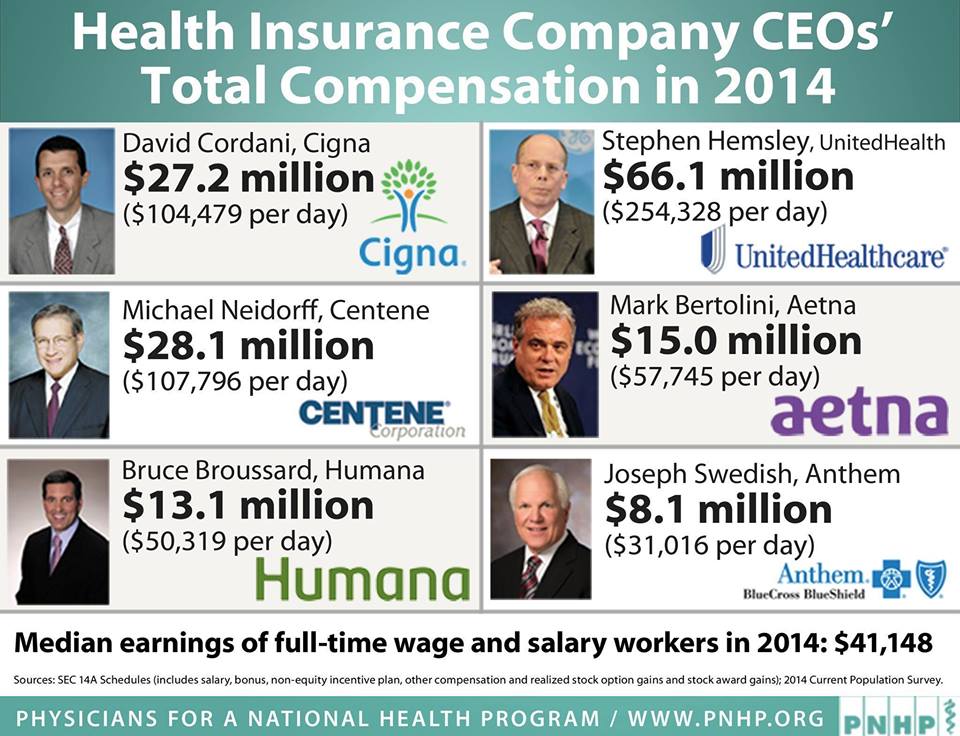
- Imposed on providers: time and staff to argue about coverage and treatment and reimbursement.
- Lack of standards: providers and patients have to use plans and forms specific to each company.
- Bad actions: bias toward denying coverage, pressing for minimal reimbursement, deceptive plans.
- Company costs: profit, high executive salaries, advertising, lobbying, lawyers.
- Costs imposed on society or economy in general:
- Bankruptcy of patients when they are uninsured or under-insured.
- Reduced productivity (sick workers).
- Increased chance of epidemics (caused by sick people).
- Uninsured:
- Lack of access.
Schoen, Osborn, Squires, and Doty's "Access, Affordability, and Insurance Complexity Are Often Worse in the United States Compared to 10 Other Countries" - Errors.
- Medical problems due to preventable causes (accidents,
lack of preventive care, drug and alcohol abuse, etc).
From Wikipedia's "Health care in the United States" 2013:
The United States life expectancy of 78.4 years at birth, up from 75.2 years in 1990, ranks it 50th among 221 nations, and 27th out of the 34 industrialized OECD countries, down from 20th in 1990. Of 17 high-income countries studied by the National Institutes of Health in 2013, the United States had the highest or near-highest prevalence of infant mortality, heart and lung disease, sexually transmitted infections, adolescent pregnancies, injuries, homicides, and disability. Together, such issues place the U.S. at the bottom of the list for life expectancy. On average, a U.S. male can be expected to live almost four fewer years than those in the top-ranked country.
According to the World Health Organization (WHO), the United States spent more on health care per capita ($8,608), and more on health care as percentage of its GDP (17.9%), than any other nation in 2011. The Commonwealth Fund ranked the United States last in the quality of health care among similar countries, and notes U.S. care costs the most.
The U.S. Census Bureau reported that 49.9 million residents, 16.3% of the population, were uninsured in 2010 (up from 49.0 million residents, 16.1% of the population, in 2009). A 2004 Institute of Medicine (IOM) report said: "The United States is among the few industrialized nations in the world that does not guarantee access to health care for its population." A 2004 OECD report said: "With the exception of Mexico, Turkey, and the United States, all OECD countries had achieved universal or near-universal (at least 98.4% insured) coverage of their populations by 1990." A 2010 report observed that lack of health insurance causes roughly 48,000 unnecessary deaths every year in the United States. In 2007, 62.1% of filers for bankruptcies claimed high medical expenses. A 2013 study found that about 25% of all senior citizens declare bankruptcy due to medical expenses, and 43% are forced to mortgage or sell their primary residence.
From Steven Brill's "Bitter Pill: Why Medical Bills Are Killing Us" (PDF) 2013:
... In the U.S., people spend almost 20% of the gross domestic product on health care, compared with about half that in most developed countries. Yet in every measurable way, the results our health care system produces are no better and often worse than the outcomes in those countries.
... We may be shocked at the $60 billion price tag for cleaning up after Hurricane Sandy. We spent almost that much last week on health care. ...
... America's largest city may be commonly thought of as the world's financial-services capital, but of New York's 18 largest private employers, eight are hospitals and four are banks. Employing all those people in the cause of curing the sick is, of course, not anything to be ashamed of. But the drag on our overall economy that comes with taxpayers, employers and consumers spending so much more than is spent in any other country for the same product is unsustainable. Health care is eating away at our economy and our treasury.
The health care industry seems to have the will and the means to keep it that way. According to the Center for Responsive Politics, the pharmaceutical and health-care-product industries, combined with organizations representing doctors, hospitals, nursing homes, health services and HMOs, have spent $5.36 billion since 1998 on lobbying in Washington. That dwarfs the $1.53 billion spent by the defense and aerospace industries and the $1.3 billion spent by oil and gas interests over the same period. That's right: the health-care-industrial complex spends more than three times what the military-industrial complex spends in Washington.
From bigfish42 (Masters student in healthcare administration) on reddit:
> What caused American medical prices to be so obscenely high?
There's been a ton of research on this, and there are at least five big drivers: Waste, Price Insensitivity, Technology, Market Pressures, and Regulation.
Something like 30% of our health spending is pure waste. Well, worse than pure waste because of the risk of negative outcomes (hospital-acquired infections, death, etc). This can be from all kinds of things, from outright fraud to doctors and systems simply covering their butts, to doctors agreeing to treatments that patients asked for so they don't lose their future business.
If you understand supply/demand models, I hope that you know a bit about price sensitivity. There is an assumption of a downward sloping demand for healthcare services with respect to price paid (higher cost -> less demand for it). The trouble is that the payor is not the same as the recipient of the service, and neither is the one who makes the recommendation. Here, the one that recommends the treatment is often the one who gets paid for doing things (the doc), the one who pays often just gets a bill for what has been done (the insurer), and the one who receives the service (the patient) just pays their copay - a cost that has little to do with the total price of the service.
A huge driver of costs is the "arms race" of the latest technology. This has all kinds of drivers that are worth diving into - like our current patent and approvals process ... The consequence is that doctors and health system spend a massive amount of money on new technology that patients demand that has little (if any) positive effect on outcomes.
In terms of market structure, there is massive fragmentation among providers. And they are the ones who have to buy supplies. Since there isn't one big purchaser of supplies (including meds, devices, durable medical supplies, etc) and there are just a few major players for specialized (and patented) supplies, the providers have little bargaining power to keep costs of supplies down. The higher costs from less market power get passed on to customers. Additionally, consumers - patients - don't have any real power, except through their insurers, to keep costs down. (But if there exists a patients' union, let me know!)
Finally, regulation. It costs a lot of money to comply with all of the regulations. This goes from staffing (doctor training is massively expensive and heavily regulated), to job designation (there is generally a very well-defined scope where an individual can practice), to required emergency care (see EMTALA) driving up the cost of bad debts, and even to requirements related to safety. These all cost a lot of money, and those costs all get factored in when the providers set their prices. With the general price insensitivity, and lack of customer power, these costs generally go straight through to increase the cost of care.
It's messy, but those are the top 5 IMO.
From AlexFromOmaha on reddit:
> How is hip replacement in Spain instead of USA
> so much cheaper there?
It's not exactly labor costs or profit margins, but it's primarily those two rolled into one.
The labor overhead of an American hospital is substantially higher. A single-payer health system costs significantly less administratively. The private insurance system takes a legion of specially-trained medical coding and billing specialists trying their level best to extract the highest negotiated prices from insurance companies, and the insurance companies respond by having departments literally devoted to finding excuses to refuse claims. Then the hospital will send the bill for the aggressively and expensively classified service to the patient first, because all they saw was "claim denied", and no one is about to admit wrongdoing or confusion by the whole cumbersome thing that's way worse than you think. This makes the patient unhappy, and the patient is a customer, and the US believes in customer service in a way you won't find anywhere else. Now you have the patient advocacy departments, both in the hospitals and the insurance companies. All of these people are expensive. None of them are minimum-wage laborers. None of them add actual value to your healthcare. They exist to extort or save money in a corporate arms race.
Also, in true American fashion, the business is business, and business is good. The executives of healthcare anything, whether it's hospitals, insurance companies, or healthcare-related manufacturers, they get paid orders of magnitude more than their European counterparts. In the US, no one says, "Wait, they're not the specially trained experts, they're just businessmen, why do they make so much more than doctors?" They say, "Of course managers make more than their employees, and the directors make more than managers, and the VPs make more than the directors, and the presidents make more than the VPs, and the C*Os make more than them. How else would we get people to do the job?"
Depending on who you ask, you could drop healthcare costs in the US by 10-40% just in labor reductions by switching to a single-payer system. (I think the honest reality is that, since we have a legion of medical coders at the ready and no one would let a good corporate weapon go to waste, so you'll see the fight move to hospitals v government, and the low end of that scale is correct.)
Then you have the costs. Ye gods, the costs. Here's where you get the profit margins.
Prescription drugs are a big one. I'm all for drug patenting, but drug companies level absolutely insane costs for drugs with no generics, and they'll go to great lengths to find new ways to patent the same drug. Just because they're the worst doesn't mean that they're the only ones. High-end medical equipment has the same patenting and cost issues. Then there's all the lab supplies and reagents, run-of-the-mill equipment, lubricants, tubes, and assorted sundries meant for hospitals. Those manufacturers, they all get paid well.
Then there's the approach. If you have chronic high cholesterol, an American doctor will prescribe you a statin and hand you a pamphlet on lifestyle changes you might consider making. A Spanish doctor will call you a fatty, put you on a diet and send you jogging for a few months, and maybe if that doesn't work you'll get a prescription.
Then there's you, the average American healthcare consumer. You have no idea what dollar amounts are being thrown around if you have an insurance with co-pay. You probably don't know that the anti-nausea medicine you're taking costs almost $100 a pill, or the Advair that only helps your asthma a little costs fifty times more than the albuterol that'll save your life in a pinch. You don't go price-shopping hospitals or refusing silly services that'll cost your insurance company hundreds of dollars. You go, get care, leave, and let the rest of that happen behind the scenes. There's no downward pressure on these prices, so they'll continue to inflate.
EDIT: I totally forgot about "preventative care", the newest fad in healthcare extortion. Outside the US, preventative care means a nice sit-down with a dietitian and a daily stroll. In the US, this $2500 test can make a disease cost $6000 to treat instead of $150,000! Great deal! So let's get fifteen million people to get this test every year to prevent two thousand cases for a net savings of negative thirty-seven billion dollars. In some cases (mammograms and colonoscopies are the most visible examples here, but not the only), this results in over-intervention. Things that would resolve themselves are instead treated aggressively.
Hi, Economist here (worked on healthcare costs for about 10 years starting in 2002): KINDA.
Single-payer IS better and cheaper. You present a pretty good summary, but you do get some things wrong. There is, OF COURSE, downward pressure on prices ... from the insurance companies paying those prices. "$100 a pill" is a meaningless (in most cases) "MSRP" number. It's what you might "pay" with no insurance assuming you actually paid your medical debt at 100% of the billed value. It isn't what insurance companies pay.
...
Also, while over-screening is absolutely a problem in the US (mammograms are ludicrously over-utilized for screening when they should likely be primarily a diagnostic tool), the stereotype of "let's eat right and exercise and see what happens" from Euro docs and "let's take this pill, get this scan and cut that f**ker out" from US docs is greatly exaggerated.
It sounds great, but the reality is that European citizens also take lots of drugs, ignore docs advise and have adverse outcomes. I worked a lot on cancer. You know who gets a lot of cancers per capita? France, Belgium, Denmark, Norway. All at a higher rate than the US (where, incidentally, because of the over-screening previously mentioned, there is likely some rate-inflation of "borderline" cancers that don't require much treatment.)
Some health outcomes are better in Europe or Canada, some aren't. The US is an amazingly demographically diverse place. Health outcomes for wealthy people in the US are great. Health outcomes for poor people in the US are borderline catastrophic. That's a problem, but the idea that it's all greed and profit motive causing the issue with the poor people is an empty correlation for the most part. Single-payer healthcare would help with poor people's health outcomes, but almost without question not as much as removing them from poverty would. Cheap good healthcare is great for health outcomes, not living life under crushing stress is far better.
As I say, it's complicated.
Nearly Right's "American hospitals charge uninsured patients 500% above Medicare rates whilst AI tools expose systematic fraud"

From Rachel Pearson's "Texas' Other Death Penalty" 11/2013:
There's a popular myth that the uninsured - in Texas, that's 25 percent of us - can always get medical care through emergency rooms. ... The myth is based on a 1986 federal law called the Emergency Medical Treatment and Labor Act (EMTALA), which states that hospitals with emergency rooms have to accept and stabilize patients who are in labor or who have an acute medical condition that threatens life or limb. That word "stabilize" is key: Hospital ERs don't have to treat you. They just have to patch you up to the point where you're not actively dying. Also, hospitals charge for ER care, and usually send patients to collections when they cannot pay.
From Jeramiahh (worked in Medical billing and insurance for 5 years, plus Medicare.gov) on reddit 1/2017:
Medicare is a national, publicly-funded medical insurance, divided into three parts: A, B, and D. While technically available to purchase under the age of 65, the cost is unreasonable (if I recall, $400/mo per person, for each part), therefore, the vast majority of people with Medicare are aged 65+, who have paid into it through their taxes, for a minimum of 10 years. Part A is received for free, and covers Inpatient (ie; in-hospital) charges; stays, surgeries, etc. Part B is Outpatient, such as visiting your doctor for checkups. Part D is pharmacy coverage. There is also Part C, called Medigap, offered by commercial entities; for a premium, they cover things that Medicare does not. Medigap is designed for people with fixed incomes (ie, retirees), as it smooths out the cost of medical care; they pay a large premium each month, but little or nothing if they need medical services. Part A is offered for free, Part B costs $150/mo, per person, Part C varies depending on coverage, but ranged from $50-150/mo, and Part D is often offered as part of Part C plans, also from commercial entities.
Medicaid, on the other hand, is medical coverage for those without the resources to afford more. It is funded by the state, as opposed to by the nation, and its benefits will vary from state to state, but in general, it is only available for those in severely disadvantaged circumstances; disabled, poverty, orphaned children, etc. It has little, or often no, monthly premium, and offers extreme reductions in costs of medical bills, often 90-95% or more.
For more details on how health insurance works, it's a little complicated, which is, honestly, intentional, to confuse people. Health insurance is made up of several major components: The premium, or what you pay each month, the Deductible, or what you pay before the insurance company does, the Copayment, or what you pay, regardless of deductible, for a service, the Coinsurance, or what percentage of the service the insurance company pays, and the Out Of Pocket Maximum, or how much you will pay, in a worst-case scenario, each year. Also note that insurance companies negotiate with the doctor, and lower the costs of services.
The easiest ways to discuss these is to look at various types. For this example, I'll use a High Deductible plan, a High Premium plan, Medicare, and Medicaid, to lay out the examples.
A High deductible plan might have a premium of $100/mo, a Deductible of $5000, a Copay of $20, a Coinsurance of 85%, and an OOP Max of $10,000
A High Premium plan might have a premium of $250/mo, a Deductible of $1500, a Copay of $10, a Coinsurance of 90%, and a OOP Max of $3000
Medicare (Part B) has a premium of $150/mo, a Deductible of $150, a Copayment of $0, and a Coinsurance of 80%, with no OOP Max.
Medicaid might have a premium of $0, a Deductible of $0, a Copayment of $2, a Coinsurance of 95%, and no OOP Max.
Finally, you have no insurance. It's free, but under the ACA, if you choose to not have any insurance, you pay a fine of several hundred dollars. I don't know what it is offhand.
So, let's say you need to visit a doctor, for a regular checkup visit. The doctor charges $150 for this services.
Under the High Deductible plan, the doctor bills the $150. The insurance then negotiates it down to $110, cutting that $40 off the top. You pay the Copay in the office, that day, of $20. The insurance determines you haven't met your deductible, so they remove the remaining $90 from your deductible, leaving $4,910 for the year. You then receive a bill for the remaining $90.
Under the High Premium plan, the doctor bills the $150. The insurance then negotiates it down to $100, cutting that $50 off the top. You pay the Copay in the office, that day, of $10. The insurance determines you haven't met your deductible, so they remove the remaining $90 from your deductible, leaving $1,910 for the year. You then receive a bill for the remaining $90.
Under Medicare, the doctor bills the $150. Medicare negotiates it down to $75, cutting it in half. You do not have a copay. Medicare then determines you have a $150 deductible, and removes the $75 from that, leaving $75 for the year. You then receive a bill for the remaining $75.
Under Medicaid, the doctor bills the $150. Medicaid negotiates it down to $35, reducing it by $115. You pay a $2 copay that day. Medicaid does not have a deductible, so they pay 90% of the remaining $33, or $30. You receive a bill for $3 more.
You have no insurance. You pay $150.
Two months later, you go in for a series of tests, x-rays, and eventually outpatient surgery. This is expensive, but does not require hospitalization. The doctor charges $4000 for these services.
Under the High Deductible plan, the doctor bills the $4000. The insurance then negotiates it down to $3300, cutting that $700 off the top. You pay the Copay in the office, that day, of $20. The insurance determines you haven't met your deductible, so they remove the remaining $3280 from your deductible, leaving $1630 for the year. You then receive a bill for the remaining $3280.
Under the High Premium plan, the doctor bills the $4000. The insurance then negotiates it down to $3000, cutting that $1000 off the top. You pay the Copay in the office, that day, of $10. The insurance determines you have now met your deductible, so they remove the remaining $1,910 from your deductible, leaving $0 for the year. They then pay 90% of what remains, or $981. You then receive a bill for the remaining $2019, which is the $1910 from your deductible, and $109 left over from the coinsurance.
Under Medicare, the doctor bills the $4000. Medicare negotiates it down to $2700, reducing it by $1300. You do not have a copay. Medicare then determines you have met the deductible, removing $75 to pay for it. They then pay 80% of the remaining $1225, or $980. You then receive a bill for $320, which is the $75 deductible, plus the 20% of $245.
Under Medicaid, the doctor bills the $4000. Medicaid negotiates it down to $2000, reducing it by $2000. You pay a $2 copay that day. Medicaid does not have a deductible, so they pay 90% of the remaining $1998, or $1798.20. You receive a bill for $199.80 more.
With no insurance, you pay the $4000.
Several months later, you have a major surgery. It requires three weeks in the hospital, and is very expensive, costing $100,000.
Under the High Deductible plan, the doctor bills the $100,000. The insurance then negotiates it down to $70,000, cutting that $30,000 off the top. You pay the Copay in the office, that day, of $20. The insurance determines you haven't met your deductible, so they remove the remaining $1630 from your deductible, leaving $0 for the year. They then pay at 85% of the remaining $68,350, or $58,097.50. You then receive a bill for only $6,630, which is $10,252.50 plus $1630... but you met your Out of Pocket Maximum of $10,000 for the year, so they put a hard cap on it, and paid the remaining $5,252.50 at 100%.
Under the High Premium plan, the doctor bills the $100,000. The insurance then negotiates it down to $80,000, cutting that $20,000 off the top. You pay the Copay in the office, that day, of $10. The insurance determines you've met your deductible, so they then pay at 90% of the remaining $79,990, or $71,991. You then receive a bill for only $871, since you've now hit your $3000 Out of Pocket Maximum. Your insurance covers everything remaining, which would have been over $7000.
Under Medicare, the doctor bills $100,000. Medicare negotiates it down to $72,000, cutting off $28,000. It then pays 80%, since you have no copay, and met your deductible, or $57,600. You receive a bill for $14,400. (As a side note, I did not work in Hospital billing, so this may be inaccurate for Part A, but it's a good example nonetheless. I believe Part A and Part B have separate deductibles, but I'm nearing the post limit).
Under Medicaid, the doctor bills $100,000. Medicaid reduces it to $45,000, cutting off $55,000. They pay 95% of it, or $42,750. You receive a bill for $2,250, and likely have to declare bankruptcy.
Under no insurance, you receive a bill for $100,000, and declare medical bankruptcy.
As a side note, if you have Medicare Part C, and a strong one, you likely would not receive a bill, at all, for any of the Medicare portions.
Total costs of premium + costs:
High Deductible: $11,200
High Premium: $6,000
Medicare: $16,595
Medicaid: $2454.80
No insurance: $104,150 + ACA fine
[Some of my numbers may be out of date, I'm writing all of this from memory.]
From comment by Sure 9/2022 on article:
The US does not have a healthcare system. It has several. Medicare is single-payer option with overwhelmingly private provision and some alternative administrative choices with a thick skim of secondary overlays of private health insurance. The Indian Health Service is full Beveridge. Kaiser is a single private system with nearly full vertical integration. Tricare is a social insurance model with limited private provision. Employer-based healthcare is privately funded (with a generous tax break on said provision), privately administered (subject to millions of pages of regulation), and privately provisioned (with minor exceptions for state-funded hospitals and the like). Then we have health sharing which are explicitly not health insurance, but involve "voluntary" assumption of costs by members, often linked by religious belief.
Then you have the growing cash-healthcare option where providers take all comers, but only those who can put cash on the barrelhead because the paperwork is too expensive. And of all the ways healthcare is administered in this country, this and the VA are the only ones that do not run the full gamut of provision (at least not yet).
I have worked for most of these. All of them are larger systems than multiple small European countries. All of them are wildly more expensive than similar mechanisms of provision overseas. All of them suffer from intrusive, expensive meddling by politicians and bureaucrats that result in active degrading of patient care in my experience.
My response to "insurance companies are not the problem"
The health-insurance industry is a parasite that keeps us from fixing our healthcare system (from even understanding the costs and behavior, in some cases). We need to eliminate it.
Insurance companies affect the whole healthcare system. Insurance industry costs include more than just the money that goes directly to them. That money is "only" 4% of total healthcare dollars (but 4% of a bazillion still is a big number, worth saving). But the insurance industry imposes massive time and money costs on providers (doctors, hospitals, etc) and patients and employers. Providers have to hire staff to deal with insurance, doctors have to spend time negotiating care with insurance reps, bills go back and forth multiple times as things get negotiated. Forms and rules and paperwork is different for each company and each plan. Effort is spent in cost-shifting, maintaining different price lists for different classes of patients. And by making the whole system more complex and opaque, the system becomes harder to analyze and fix. Getting rid of the health insurance industry would simplify everything.
There's also the "friction" that changing from one insurance company to another would impose, if you changed jobs or moved to a different state. And the lobbying of politicians.
Some relatively easy "technical" fixes
- Standard forms (for claims, prescriptions, charts, patient history, lab results, etc)
used by all insurance companies, doctors, labs, hospitals, pharmacies, etc.
This would reduce costs and errors for everyone.
Ryan Cooper's "The most underrated argument for single-payer health care" - Standard number-codes for prescription drugs, which must be
written on prescription forms and patient charts (in addition to
the info already written there today). This would
reduce errors.
- Absolutely free care and supplies for simple, cheap things that prevent
more expensive complications later: vaccinations, condoms, needles, blood-pressure monitoring,
diabetes screening, smoking cessation, diet/nutrition/obesity advice, etc.
Hard / controversial / Draconian fixes
- No insurance coverage for very expensive
procedures (heart transplant, heart-lung transplant,
extremely premature birth, etc). The money used by one of these
procedures would pay for preventive or routine care for a thousand people.
- No insurance coverage for fairly expensive
procedures as a result of self-inflicted problems
(liver transplants for alcoholics, cancer operations for smokers, etc).
The money used by one of these
procedures would pay for preventive or routine care for a hundred people.
Socially hard fixes
- Educate people so they actually take their prescribed medicines properly.
- Change attitudes toward end-of-life, so that people accept palliative care (pain
and symptom management) as they head toward death, instead of demanding
extreme and costly measures.
Michael Bell's "Why 5% of Patients Create 50% of Health Care Costs" - Change attitudes toward diet and exercise and smoking.

Technology that could reduce costs
- Electronic patient-records and charts and drug ordering, with intelligence built in.
This would reduce errors, be faster than shuffling paper, reduce the administrative overhead
on doctors and nurses and pharmacists.
- A permanently-implanted chip in each person, which monitors their vital signs 24/7.
Similar to an airplane's "black box" recorders. But it also could alert you if it
detected the start of a heart attack, blood sugar level getting out of line, etc.
This data could reduce trips to the ER, speed up and give more data to patient evaluation in office or ER,
reduce the number of tests and scans needed.
- Making patient data available to the patient themselves, instead of keeping it
hidden in doctor's files. Some doctors fear the patient would misinterpret it, and
get panicked or demand additional tests or drugs. But with intelligent apps or web pages
to evaluate and interpret the data, patients could get a better handle on their health.
They might be able to catch errors in their treatment, or be alerted when it's time
to have a routine physical or some new test, based on their age. And it might be interesting
if they could compare their data to that of their siblings, to see if something genetic
needs to be addressed.
Taking a step back to look at the bigger picture
I once attended a talk by C. Everett Koop (after he left office) where he said something like:
"No one ever designed the US health-care system. It just grew, haphazardly."
Much of US health-care is employer-funded because during WW II there were controls on wages, and a shortage of workers. So employers stole workers from other companies by offering better benefits, including employer-paid health-care.
Even thinking selfishly, we can't have a totally free-market system, because that would lead to an environment we don't want: poor sick people dying on the streets, poor children with horrible avoidable diseases, epidemics starting with the poor and spreading to everyone. That's why hospital emergency rooms treat everyone today: those of us who can pay don't want what would result from a no-pay-go-away policy. That's also why we have food-banks and homeless shelters and Social Security and other programs: not just because it's a morally right thing to do, but to benefit the non-poor too. We wouldn't want to live in a totally-privatized, no-safety-nets society; it would be ugly.
Are those who are against "socialized medicine" also in favor of getting rid of the VA medical system ? It's govt-provided healthcare, as socialist as it could be.
From Phillip Carter's "How to Fix the VA":
The VA is the second-largest cabinet agency, and the nation's largest health care and benefits provider,
with an overall fiscal 2015 budget of $165 billion (greater than the State Department, USAID, and entire intelligence community combined),
including $60 billion for health care. The VA employs more than 320,000 personnel to run 151 major medical centers,
820 outpatient clinics, 300 storefront "Vet Centers", more than 50 regional benefits offices,
and scores of other facilities. This massive system provides health care to roughly 9 million enrolled veterans,
including 6 million who seek care on a regular basis.
Parts of a health-care system
- Participants / patients (may be voluntary, universal, and grouped or not).
- Payers (may be single-payer/government, employers and/or individuals).
- Insurance companies (aggregate money and risks).
- Service providers (hospitals, clinics, doctors, nurses, home care workers, consultants, educators).
- Services (always rationed, in some way: by money, long waiting lists, limited
facilities, or explicit policy by insurance plan or provider).
- Material providers (pharmaceutical companies).
Some linkages
- More participants (especially universal) and fewer payers (especially single-payer) can lead to
economies of scale in purchasing materials (drugs) because of more leverage when negotiating
with the drug companies.
- Fewer payers (especially single-payer) can lead to
reduced administrative overhead because of fewer forms, fewer insurance companies to contact,
fewer policies to understand.
- More participants (especially universal) can lead to economies of scale in service providers (bigger hospitals, more clinics).
Having some people go uninsured is bad because
- Uninsured sick people can infect insured people.
- Uninsured people let easily-treated conditions mature into expensive emergencies later,
and we all pay for those emergencies.
- Uninsured people can have damaged babies,
and we all pay for lifetime care of those babies.
- Uninsured people go bankrupt when they have a major medical emergency,
and we all pay for those bankrupcties.
- Young healthy people will choose to stay uninsured, so the "average health" of those in insurance will be worse, meaning higher average cost of insurance.
- Uninsured people are part of society and part of the workforce; businesses and all of us get
reduced services when they get sick.
A universal-participants, single-payer system would tend to reduce the amounts of money spent by drug companies on lobbying and advertising, reducing costs for everyone.
From Steffie Woolhandler and David Himmelstein's "Why Obama's Public Option Is Defective, and Why We Need Single-Payer" 7/2009:
[Written while ACA was being debated in Congress in 2009, and addressing the question of whether a system can be half private-insurance and half public-payer (the "public option"):]
The president's health plan can't make universal, comprehensive coverage affordable.
Only single-payer health reform "Medicare for All" can achieve that goal.
Single-payer national health care could realize about $400 billion in savings annually - enough to cover the uninsured and to upgrade coverage for all Americans. But the vast majority of these savings aren't available unless we go all the way to single payer.
A public plan option might cut into private insurers' profits. That's why they hate it. But their profits - roughly $10 billion annually - are dwarfed by the money they waste in search of profit. They spend vast sums for marketing (to attract the healthy); demarketing (to avoid the sick); billing their ever-shifting roster of enrollees; fighting with providers over bills; and lobbying politicians. And doctors and hospitals spend billions more meeting insurers' demands for documentation.
A single-payer plan would eliminate most insurance overhead, as well as these other paperwork expenses. Hospitals could be paid like a fire department, receiving a single monthly check for their entire budget. Physicians' billing could be similarly simplified.
With a public insurance option, by contrast, hospitals and doctors would still need elaborate billing and cost-tracking systems. And overhead for even the most efficient competitive public option would be far higher than for traditional Medicare, which is efficient precisely because it doesn't compete. It automatically enrolls seniors at 65 and deducts their premiums through the social security system, contracts with any willing provider, and does no marketing.
Health insurers compete by NOT paying for care: by seeking out the healthy and avoiding the sick; by denying payment and shifting costs onto patients; and by lobbying for unfair public subsidies (as under the Medicare HMO program). A kinder, gentler public plan that failed to emulate these behaviors would soon be saddled with the sickest, costliest patients and the highest payouts, driving premiums to uncompetitive levels. To compete successfully, a public plan would have to copy private plans.
Decades of experience teach that private insurers cannot control costs or provide families with the coverage they need. And a government-run clone of private insurers cannot fix these flaws.
Tom Tomorrow cartoon2
Good articles:
Frontline's "Health Care Systems - The Four Basic Models"
On AlterNet, by Sarah Ruth van Gelder and Doug Pibel
PNHP's "Single-Payer Myths; Single-Payer Facts"
Ezra Klein's "Why an MRI costs $1,080 in America and $280 in France"
Josh Barro's "Here's Why Both Parties Lie All the Time About Health Care"
Josh Barro's "Here's Why Health Insurance Is So Weird"
Michael Goodwin's "Obamacare: what it is, what it's not"
The new Massachusetts system, as I understand it
- Participants: Everyone is forced to participate, with non-poor being forced to pay premiums.
- Payers: government pays for the poor, employers and individuals pay for the non-poor.
- Insurance companies: not sure, policies are being bundled together somehow, but still run privately.
- Service providers: no change: hospitals, clinics, doctors, nurses, consultants, educators.
- Services: no change: always rationed, in some way.
- Material providers: no change.
The proposed new California system, as I understand it (very similar to the new Massachusetts system)
- Participants: Everyone is forced to participate, with non-poor being forced to pay premiums.
Illegal alien children are covered too.
- Payers: government pays for the poor, employers and individuals pay for the non-poor;
many more employers forced to pay for coverage for employees.
- Insurance companies: still private, but administrative costs are capped.
- Service providers: no change: hospitals, clinics, doctors, nurses, consultants, educators.
- Services: no change: always rationed, in some way.
- Material providers: no change.
Smart people (including my Mom) say the answer is "Medicare for everyone", which means
- Participants: Everyone is forced to participate.
Not sure about illegal aliens.
- Single-payer: government pays for everyone. Very efficient; Medicare has very low administrative costs.
- Insurance companies: only for supplemental coverage for things not covered by Medicare, or people and providers who
choose to stay outside Medicare.
- Service providers: no change: hospitals, clinics, doctors, nurses, consultants, educators.
But many do not accept Medicare's rates.
- Services: rationed by Medicare rules, unless you go outside the system.
- Material providers: rationed by Medicare rules, unless you go outside the system.
Health-care costs (Medicare and Medicaid) in the federal budget are ballooning. Some fixes:
- Let Medicare negotiate for bulk-purchase drug-price discounts. Forbidden by law
right now. Medicaid is allowed to negotiate, and gets big discounts.
- Better coordination of patients who get both Medicare and Medicaid, and have multiple chronic conditions.
- Co-pays so patients have an incentive to avoid unnecessary procedures.
- Means-testing for premiums and benefits.
- More standardization of forms and terms and treatments, to reduce costs and errors.
- More patients into the system (best: universal coverage), to increase standardization and economies
of scale. Also would increase number of patients who get routine preventive care, thus reducing the
number who suddenly show up at the emergency room with severe problems.
'Medicare for All' Would Cover Everyone, Save Billions in First Year
Rose Roach's "Counterpoint: We want true Medicare for all, not today's semi-privatized mess"
From Robert Reich's "The Hoax of Entitlement Reform":
The underlying problem is the soaring costs of health care - as evidenced by soaring premiums, co-payments, and deductibles that all of us are bearing - combined with the aging of the boomer generation.
The solution isn't to reduce Medicare benefits. It's for the nation to contain overall healthcare costs and get more for its healthcare dollars.
We're already spending nearly 18 percent of our entire economy on health care, compared to an average of 9.6 percent in all other rich countries.
Yet we're no healthier than their citizens are. In fact, our life expectancy at birth (78.2 years) is shorter than theirs (averaging 79.5 years), and our infant mortality (6.5 deaths per 1000 live births) is higher (theirs is 4.4).
Why? Doctors and hospitals in the U.S. have every incentive to spend on unnecessary tests, drugs, and procedures.
For example, almost 95 percent of cases of lower back pain are best relieved by physical therapy. But American doctors and hospitals routinely do expensive MRI's, and then refer patients to orthopedic surgeons who often do even more costly surgery. There's not much money in physical therapy.
Another example: American doctors typically hospitalize people whose diabetes, asthma, or heart conditions act up. Twenty percent of these people are hospitalized again within a month. In other rich nations nurses make home visits to ensure that people with such problems are taking their medications. Nurses don't make home visits to Americans with acute conditions because hospitals aren't paid for such visits.
An estimated 30 percent of all healthcare spending in the United States is pure waste, according to the Institute of Medicine.
We keep patient records on computers that can't share data, requiring that they be continuously rewritten on pieces of paper and then reentered on different computers, resulting in costly errors.
And our balkanized healthcare system spends huge sums collecting money from different pieces of itself: Doctors collect from hospitals and insurers, hospitals collect from insurers, insurers collect from companies or from policy holders.
A major occupational category at most hospitals is "billing clerk". A third of nursing hours are devoted to documenting what's happened so insurers have proof.
Cutting or limiting Medicare and Medicaid costs, as entitlement reformers want to do, won't reform any of this. It would just result in less care.
In fact, we'd do better to open Medicare to everyone. Medicare's administrative costs are in the range of 3 percent.
That's well below the 5 to 10 percent costs borne by large companies that self-insure. It's even further below the administrative costs of companies in the small-group market (amounting to 25 to 27 percent of premiums). And it's way, way lower than the administrative costs of individual insurance (40 percent). It's even far below the 11 percent costs of private plans under Medicare Advantage, the current private-insurance option under Medicare.
Healthcare costs would be further contained if Medicare and Medicaid could use their huge bargaining leverage over healthcare providers to shift away from a "fee-for-the-most-costly-service" system to a system focused on achieving healthy outcomes.
Medicare isn't the problem. It may be the solution.
Some call universal health-care or government-paid health-care "socialism". But how does it differ from public education, or public police/fire/EMS/hospitals/sanitation, or public roads ? If something is a public good, and perceived as essential to basic public needs, and best run or paid for by the government, the public approves of it.
This Modern World on healthcare
Answer to the "mandates are un-Constitutional" argument:
Eliot Spitzer's "Originalist Sin"
From someone on reddit:
I've worked as an ER nurse in the US for the last 18 years. The system does suck.
I have the skills to:
- Help a doctor do an emergency thoracotomy (cut a person's chest open) and plug a hole in a person's heart with a finger in less than 4 minutes.
- Help a neurosurgeon drill a hole in someone's brain in the ER.
- Repack someone's colon when it has prolapsed out of their anus.
- Stick an IV needle into the vein of a screaming two year old who is dying of sepsis in the first try.
- Drill an IV into the bone marrow of your tibia if you are dying and the paramedics couldn't get an IV in you.
- Resuscitate a newborn that died in childbirth.
- Pack and preserve your severed arm long enough for them to reattach in the OR.
- Stick an occlusive dressing on your sucking chest wound seconds after walk into triage after some ass-hat just shot you in a drive-by.
- Replace your entire blood volume twice over in 27 minutes while you have a massive hemorrhage because you parked your car into a telephone pole at 120 mph.
- Shock you with 300 joules within seconds of you heart going in to a lethal arrhythmia.
- Quickly scan a waiting room full of screaming children in a pediatric trauma center, and figure out which of the 60 waiting babies might die and which can wait in line 24 hours to see the doctor.
But, most of my time, is making sure that I don't have to do all these things.
And, while I've done every single thing on the above list, most of my time is spent taking care of ear aches, sore throats, flu symptoms, alcoholics who drank too much, and passed out soaked in their own urine on a park bench, or people who have coughs, a fever and chills who really should just stay home and take some Tylenol. We also deal with an immense number of drug addicts who try to game the system and weasel a prescription for narcotics out of the doctor.
Yes, unless you are near death, our health care system sucks. At that point, you get some of the best, quickest care in the world. It doesn't just suck for you. It sucks for us working in the system as well.
From someone on reddit 2012:
In Texas, we had very thorough malpractice reform more than a decade ago.
Lawsuits dropped, settlements are capped, and medical care and insurance costs keep going up and up and up.
Ben Sherman's "STUDY: Texas Tort Reform Did Not Reduce Health Care Costs"Julie Rovner's "Costs Of Defensive Medicine May Be Overstated"
Jason Millman's "Study: Don't expect big health-care savings from medical malpractice reform"

From someone on reddit 2012:
> This is why your healthcare is so "cheap" in France.
> You have the third highest tax rate in the world
> (as of 2005).
Do me a favor. Compare tax rates of the two countries. America's is lower ? Sure. Now add the obscene amounts of money Americans spend on insurance, higher education, etc. We're not saving any money; we're merely ensuring that profit-motivated entities provide our care.
It amazes me that people think corporations are a better alternative than the government. The government is not perfect, but it's also not motivated solely by profit.
From johnnyfresno on reddit 3/2011:
... Most Americans don't hate universal healthcare, we just don't understand it. We are told that by having a public health care system, we will be paying for the health care of the poor and unemployed people, and this frightens and angers us. We fail to realize that we currently do pay for the health care of the poor and unemployed. We are told that if we have a public health care system, the big bad gubment will be making life or death decisions for us, and this angers and frightens us, but we fail to realize that these same decisions are currently being made by an organization that sees us only as a cost or revenue. We are told that in a public health care system, we will lose our ability to have choice, and this frightens us and angers us. We fail to realize that we currently are at the mercy of those who decide where and when we are treated, and those in some HMO's have almost no choice at all. We are told that in a public health care system, our taxes will increase, and this angers and frightens us. We fail to realize that our cost for health care will actually decline below current levels.
small correction. we currently do not pay for health care for the poor and unemployed. we pay for emergency care that they default on. the poor and unemployed largely do not receive any sort of health care unless they are disabled and receive medicare (some may qualify for medicaid through their state).
i support universal health care, but let's not fool ourselves. we would definitely have to expand the scope of who is covered if we implemented government run universal healthcare here.
What, and start handing out cheap preventative care instead of paying huge amounts of money for emergency care? Dear god, that'd be terrible! That would even reduce the suffering of these poor people! We can't be having any of that!
Yeah, I suppose, although I don't really pay for health care either. I don't go to the doctor unless I am sick because I don't want to pay the deductible or co-pays unless I have to. This means, I rarely engage in any preventative care. Also, my insurance won't cover "non-essential" check-ups like periodic PET scans or cardiac monitoring, even though my profession puts me at higher risk for heart issues and cancer.
Robin Zlotnick's "Former Health Insurance Exec Admits Lying to Americans About the Canadian System"
From xtachx on reddit 3/2011:
Canadian here but lived in US for a long time. ... Trust me, healthcare in Canada is 1000x better than US.
We may have higher taxes, higher car insurance, higher phone bills ... but the healthcare system makes up
for all of it. I would rather pay more taxes for free healthcare than buy toys with the money.
From lendrick on reddit 3/2011:
American here. I had to watch my wife writhe in pain from a kidney infection for five hours before they
let us into the ER, and another two hours before anyone actually treated her. Anyone who tells you
that the lines are longer in Canada is full of sh*t.
And yes, we're both insured.
From rbnc on reddit 3/2011:And yes, we're both insured.
Having an American-style healthcare system is something UK politicians threaten
the electorate with as though it was a punishment.
"If you vote for blah blah, we'll end up with an AMERICAN STYLE HEALTH SERVICE".
From flatlander30 on reddit 3/2011:"If you vote for blah blah, we'll end up with an AMERICAN STYLE HEALTH SERVICE".
Yup, same thing in Canada.
Harper wants to PRIVATIZE YOUR HEALTHCARE etc.
From FerociousImbecile on reddit 3/2011:Harper wants to PRIVATIZE YOUR HEALTHCARE etc.
"In Canada you DIE waiting for an MRI!" No, but in Canada you can wait a while for a free MRI for your bum knee
you f**ked up playing tennis while people with cancer use the machines, OR you can pay to have an MRI right away.
Unfortunately I've known 3 people who've been diagnosed with cancer over the past 5 years, and they were all
treated immediately and are thankfully in remission and at home (they didn't have to mortgage them) with NO BILLS TO PAY.
From GeneticSpecies on reddit 3/2011:
I'm a Brit living in the US. I have found the health care in the US to be about the same as the UK. Certainly not better.
We have really good insurance, and yet still have to pay co-pays, and have also spent $100's on what the insurance won't cover.
NHS rocks.
From swedish_libertarian on reddit 3/2011:We have really good insurance, and yet still have to pay co-pays, and have also spent $100's on what the insurance won't cover.
NHS rocks.
I like our universal healthcare in Sweden, but it could use some reform. If you're not pushy and somewhat well-read
you'll die in queues here (also not completely true, but too close to the mark to be comfortable).
Another discussion: reddit "What is the healthcare system like in countries like America, Canada, Sweeden, Denmark, Australia, etc? And how does ObamaCare compare?" 12/2013
Rick Steves' "My Readers Share Their Own European Health Care Stories" 10/2012
The Guardian's "How sick are the world's healthcare systems?" 10/2014
Tyler Heymans' "Healthcare Comparison Between The US and The UK" 1/2016

From The Week's "The problem with Medicare" 5/2011:
The Swiss solution
Switzerland has proved that it's possible to successfully overhaul an entire country's health-care system. In 1996, the Swiss re-created their system as a public-private hybrid providing universal health care through a network of private insurers. The system provides what almost everyone agrees is high-quality care, at a cost of less than 11 percent of GDP - compared with 16 percent in the U.S. How does Switzerland do it? The country requires all its citizens to take out personal health insurance, cutting employers out of the picture. Insurers offer a range of programs, and are forbidden from excluding anyone. The government provides a health-care subsidy to help those with lower incomes buy a policy - about 40 percent of the population. But deductibles are far higher than in the U.S., providing a disincentive to pursuing unnecessary treatments. Medical fees are renegotiated every year between health-care providers and insurance firms, and must be approved by local governments. "Chronic-disease management is better here," Zurich physician Edouard Battegay told The New York Times. "If you don't treat hypertension, you treat strokes. Not treating patients is expensive."
From discussion on reddit 6/2015:
> Doctors of Reddit: What do you think of your
> country's healthcare? What would you change
> if you could?
From /u/Rzztmass:
Sweden (Hematology fellow):
I think it's great. There is exactly one insurance that you have to work with and you basically never have to think about whether a patient can afford diagnostics and treatment. So you treat everyone the same, which makes things easier.
Lawsuits are starting to appear, but are still rarities. As long as you do not intentionally hurt someone, the worst that can realistically happen is a warning. Repeat offenders that are immune to teaching can lose their license though. As a doctor working at a state hospital, you do not have to worry about insurance and you are not personally liable.
Our computer systems are a pain though, think up to 5 different systems simultaneously (patient journal & medication, lab data & radiology, clinical physiology, cancer registry, anticoagulation). And I hear the surgeons have it worse..
Lots of administrative work which I would love to turf to a medical secretary, but we don't have enough of those.
Very few beds, least of all ICU beds.
But you go home at 4:30pm.
I'd get a decent IT system running, hire more staff to help with administration and open up more beds. For that, hire more nurses.
From /u/bruce_mcmango:
British GP trainee. I've worked in 8 different hospital medical/surgical specialties ranging from urology to geriatrics and two GP surgeries; one in the most socioeconomically deprived part of my city and one in the wealthiest.
Aneurin Bevan, the chap instrumental in founding the NHS, said: "Illness is neither an indulgence for which people have to pay, nor an offence for which they must be penalised, but a misfortune, the cost of which should be shared by the community". I am proud to serve these noble principles. In addition, a study in 2011 found the NHS saves more lives per pound spent than any other country apart from Ireland (among the 17 countries looked at, the U.S. was the least efficient).
When I think of my sick patients; the 30 year old who cannot walk due to cord compression secondary to metastatic malignant melanoma, the 98 year with reduced mobility and weight loss, the middle aged woman with new rheumatoid arthritis, the NHS has protected them at their most vulnerable. They get excellent levels of acute care, don't bear the brunt of the exorbitantly priced chemo/monoclonal antibodies and, in Scotland at least, have carers come into their homes up to 4 times a day to help them with their activities of daily living. For free; the same standard of care regardless of what you earn.
Having said that, I often question how long I can stay working in the NHS. The geriatricians I work with started their careers looking after patients who grew up pre-NHS. Comparing them to the patients who were born into the NHS, their expectations, nay, sense of entitlement, is profound. My perspective is that perhaps if people get something 'for free', they don't value it. The level of inappropriate demand, which is felt mainly by the gatekeeper GPs, is depressing. Drug addicts who will ask for their sick note in one breath and then tell you how they went illegally fishing in the next. The woman who asks for a house visit because she had a paper cut. The young adult who thinks that the local Tesco ought to have more gluten-free sandwiches and thinks it is your job, doctor, to do something about it. The relatives who see granny once a year and are shocked to find her frail, struggling on by in a dirty flat and demand that "something must be done" so long as it isn't done by them.
It seems to me that there are more and more - damn it, I'll call them what they are - time wasters you have to battle through in order to treat your ill patients.
Couple this with a government who understandably (given that our ageing population will cause our costs to skyrocket) want to run the service on a shoestring budget, a health secretary who seems to take pleasure in kicking the medical profession, endemic levels of understaffing - I wonder whether the NHS is sustainable at all.
I hope it is, but I'm not sure what it will look like in 25 years or if I would be able to cope with being part of it.
From /u/DocInternetz:
I'm in Brazil. I'm an MD/PhD, working with epidemiology and cost-effectiveness analyses; I work for both a public hospital and for a private insurance company. So, I feel quite confident in talking about our healthcare system ...
We have two tiered coverage: 75% of the population relies solely on the public health system, and 25% have private coverage. Private plans are regulated by a national agency: there's a standard coverage list, limits on co-pays, limits on annual price raises, and many other requirements. Service is usually good, barring focal difficulties for old unregulated plans and the like.
The public system is vastly criticized, sometimes with reason, sometimes not. I feel it's important to say it's viewed more favorably by those who actually use it than by those who don't. Overall I'd say it's a good system with some very serious "choke points". If you need a basic consultation or cancer treatment, you're absolutely going to get it in a timely manner. If however you need elective surgery or maybe an ultrasound, it's gonna take forever depending on your location. If you need urgent care, it better be really urgent, otherwise it's gonna be a long wait.
Some cities are achieving 100% primary care coverage (meaning, everyone in the city has a reference primary care team - physician, nurse, nurse technician, health agents), such as Florianopolis. Many lag behind, both for lack of funding and for lack of proper management. There's such great variability in the system, with places of internationally recognized excellence and places that should not have a license to function.
We have one of the best vaccination programs in the world, with over 95% coverage for all 26 vaccines (it's over 100% for the main ones). We have a very large transplant program, and although demand is still higher than donors, our rate of donors per million population has doubled since 2008 (7.2 in 2008, and now 14.2 in 2014). We also have the broadest HIV/AIDS program of developing nations and, one could argue, a quite successful one - I'd say we have definitely influenced global AIDS and health policy. All this is free at the point of care.
Overall, we're simply a nation aiming to provide universal care at the level the UK does, but with $800 per capita instead of $3000. I'm proud of many aspects of our system; there certainly is a lot to fix and improve, and I believe we can get there, with time and effort. Let's see.
From /u/Ulsenius:
Resident in The Netherlands. It is OK, I feel. The Netherlands has mandatory health insurance with a market dominated by 4 insurers. Health insurance premiums only cover a small part of health care costs, the rest is covered by taxes. Most hospitals are private, not-for-profit institutions. Nobody is denied important medical treatments due to financial reasons, although chronic illness still can be a financial burden on already poor patients. This means that there is no real competition between hospitals and other health care providers; consequently, the health insurers are a rather useless layer of overhead.
A large proportion of our GDP (only second to the US) is spent on healthcare. This is mainly due to high costs in long term care; like institutionalised persons, mental health care and nursing homes. We have highly trained physicians and up-to-date facilities. I think we can pride ourselves on the fact the we practise relatively common sense medicine: overdiagnosis and overtreatment is rare compared to other health care systems, we have one of the lowest antibiotic usage in Europe, for instance. The fact that we don't have a very litigious culture is probably one of the reasons; no extreme defensive medicine. Patient participation is on a rather high level I feel. I think we should improve the service level to our patients (waiting rooms, privacy, online scheduling, etc.).
What I would change is the exchange of medical information between hospitals. It still frustrates me that all the information that is available in our EMR, is printed and faxed to the place where I referred my patient to, which may even use the same EMR. Our secretaries scan said fax to upload it to our EMR. We can't assess radiological images that are made in the ER of hospitals that refer patients on a daily basis; the patient arrives with the CD-ROM. Our government should have made a better exchange compulsory years ago.
For my specific hospital: I still don't understand why, after ordering an emergency CT in the EMR, I have to make 3 phone calls (radiologist, CT technician and ER nurse) to get it done.
From /u/BlameYourDoctor:
American physician here.
America has some of the smartest, most well-trained physicians in the world and we should be #1 in healthcare. However, it seems like government and insurance companies purposely interfere with medicine and make it unnecessarily complex.
Graduating medical school and residency were easy compared to dealing with insurance companies, wondering if medications/procedures are covered, etc. I feel more like a businessman than a physician because I have been conditioned to only see the financial side of medicine, as it directly impacts my practice and paycheck.
In particular, I think the ACA has been overwhelmingly positive. But the ACA didn't address tort reform, which is why American physicians have to practice defensive medicine and constantly worry about lawsuits.
Physicians need to write the health care laws, not lawyers and businessmen. That is why America falls behind the rest of industrialized nations.
EDIT: I don't understand tort reform at all. I have much to learn.
From /u/marunga:
Health care consultant currently living in Germany here: It's average. It has it's good points (low waiting times for hospital based procedures, fairly good coverage with basic insurance) but also it's lows (loooonnng waiting times for specialist treatments, bad quality of nursing/associated healthcare professions, huge gap between 'private' and 'public' patients).
What I would change:
- Abolish the current system of private insurance for the bigger incomes (and public servants, self-employed, etc.) and bring them back into the public system. It does not make any sense to remove the best payers from a system that is based on solidarity. If you want more you can still insure you additionally for "luxuries" like privileged treatment, private rooms, etc.
- Do allow agglomeration of doctors much more freely than it is now. Make it the norm, not a rarity. The current system of "single doctor clinics" is highly ineffective and toxic to the political environment in many ways. Restore the old-eastern "poliklinik" as the norm.
- Increase the qualification (Bachelors degree/FH) for the associated health professions (nursing, paramedicine, physio and ergotherapy) and let them practice their profession not based on doctors referral. Make them an stand-alone part of the system.
- Increase the treatment range (and therefore qualification and budget) of GPs. Currently a lot of GPs only serve as prescription pushers, referral writers and sick note fillers, may it be due to qualification or budgetary concerns.
- Abolish the current system of payment for ambulatory treatment - make it effort based not quota based. Allow doctors to charge a different amount for specials but force them to offer basic appointments for the majority of the time. (You want an appointment after 6pm? No problem! This is 25€ out of your pocket.)
- For f*cks sake: START TO TRIAGE! Most German hospitals do not triage emergency patients, nearly 100% of the medical doctor's surgeries do not triage a patient.
- Punish patients: You lied to your triage nurse, told her you have heart problems because you knew you would get in directly instead of waiting for 3 hours? Bam. Huge fine for you.
From /u/RoboticElfJedi:
Australia: I'm a health policy analyst, so I've spoken to many clinicians but I'm not one.
The Australian system is excellent and we get good outcomes at a very efficient price by world standards. The system basically works as as follows:
- The federal government has a universal insurance scheme called Medicare (paid for by income tax) which pays a fixed amount for doctors visits, imaging, and pathology. Most doctors will see a patient for the amount paid by Medicare (called 'bulk billing', means the doctor visit is free to the patient), the rest require a co-payment from the patient. You choose your own doctor.
- State governments fund the public hospital system, which is available to all and is free of charge.
- The Pharmaceutical Benefits Scheme, another federal program, covers the cost of prescription drugs minus a small co-pay.
- There is a system of private health insurance, that is subsidised by the federal government, that covers elective surgery and stays in private hospitals as well as some extras like glasses and dental.
Strong points are the universality of the system - everyone is in the same boat when it comes to primary care and free access to GPs is not difficult to find, and hospitals provide good quality care without any cost to the patient. Quality of doctors and allied health professionals is very good.
Weak points are the private health insurance which in my view delivers poor value to most people, does little to relieve pressure on the public system and is the recipient of billions of dollars in subsidies that would be better spent on services in public hospitals. Lack of coverage for dental care. Out of pocket costs are increasing especially for some medical devices and allied health (dentist, physio, etc). Long waiting times for elective surgeries in the public system.
From /u/Flabby-Nonsense on reddit:
[Re: How UK enacted NHS:]
You have to understand that it's not surprising we adopted these changes in 1948 and [USA] didn't. The impact of the first and second world wars on the UK mainland left just about everyone expecting a change. The whole war really showed the class divide for what it was, with images of people living out on the street after their homes were bombed into dust, with everyone regardless of class knowing people fighting and dying abroad, with the evacuation of Children from cities to the country, where the rich saw first hand how the poor were being affected by the war.
Many in America are shocked that we voted Winston Churchill out of power after the war finished, due to how important of a war-time leader he was and how great he was at unifying the nation during it's hardest time. But a poll was done of the greatest British prime ministers of the 20th century and in that poll Winston Churchill ranked second. The person who ranked first was Clement Atlee, the man who replaced Churchill in 1945 and remained in office until 1951.
He was elected because he promised to enact every part of the Beveridge report that introduced the welfare state. The NHS, expansion of national insurance, raising of state pensions, unemployment benefits, child benefits, maternity benefits, sickness benefits, expansion of war pensions for the wounded and widowed. Infant mortality went down, life expectancy went up. Universal family allowances were introduced. Furthermore workers rights were expanded upon; entitlement to sick leave was increased, workers compensation was increased and much more.
Atlee did all these things and that's barely scratching the surface. But you never faced that opportunity, you weren't subjected to a continuous bombing campaign of your entire country that killed 60,000 people, that practically levelled our major cities, that forced mothers to send their children away to spare them the risk of the Nazi air raids, and we got off lightly compared with the rest of Europe. Had these things happened to you then America today would be a very different story
I do not bring this up because I want to start a Britain vs USA argument like the kind you see on youtube, I brought this up to make something very, very clear to you. You are being lied to. You are being told that a single payer health system is impossible, that increased workers rights is impossible, that advancement on welfare is impossible.
I'll tell you what's impossible: Doing those things after your country has experienced two major world wars with a depression in-between, try introducing those things when your country is completely bankrupt, when people are living out on the street, when most of the working population was out fighting the people that were bombing your civilians. Now that's impossible. Yet we did it.
You are living in the richest country on earth at a time when the earth as a whole has never been richer, yet the distance between the poor and the rich is increasing and no one notices, and anyone who offers a solution is told that it's not economically viable. It took us two world wars to see that inequality and try to do something, if we managed to create a welfare state out of nothing but dust and desire to change then you can create it out of gold, but you need that desire and so long as you allow people to bully your country into believing that change is too expensive then you will never have it.
It's time to stop saying that Bernie Sanders' ideas could never work. They worked 72 years ago and they'll work now, it's just a question of listening to reality.
Galen Barnett's "Five myths about health care around the world"
Laudan Aron's "Why Is the United States So Sick?"
Anya Schiffrin's "The French way of cancer treatment"
Canadian joke
